blogshub555@gmail.com
blogshub555@gmail.com
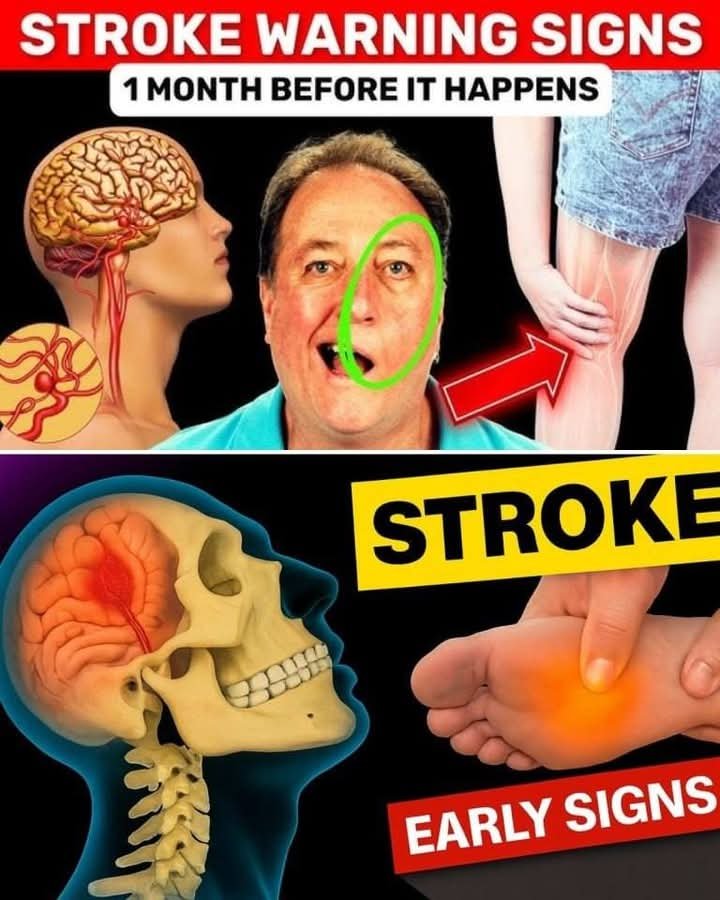
“9 signs of diabetes that appear at night,” focusing on two nighttime symptoms:
SIGNS OF DIABETES THAT SHOW UP AT NIGHT c The image highlights “9 signs of diabetes that appear at night,” focusing on two nighttime symptoms: excessive sweating and leg cramps. Below is a concise article that expands on these nocturnal warning signs of diabetes. Diabetes can sneak up on you, and some of its most telling clues show up while you’re trying to sleep. Recognizing these nighttime signals helps you catch the condition early and manage it effectively. Common night‑time diabetes symptoms1. Excessive sweating (night sweats) – Your body may release too much sweat during sleep because blood sugar swings trigger hormonal responses that raise body temperature. 2. Leg cramps or muscle spasms – High or low glucose levels can affect nerve function, causing painful cramps in the legs or feet at night. 3. Frequent urination (nocturia) – Elevated blood sugar forces the kidneys to produce more urine, waking you multiple times to use the bathroom. 4. Thirst at night – The body craps for fluids when glucose is high, leading to nighttime thirst. 5. Blurred vision – Fluctuating sugar levels can affect the eye’s lens, causing temporary vision changes after waking. 6. Restless sleep – Unstable glucose can trigger restlessness or difficulty staying asleep. 7. Morning headaches – Dehydration or sugar spikes during the night may cause headache upon waking. 8. Tingling or numbness (neuropathy) – Nerve damage from diabetes can cause nighttime tingling in hands or feet. 9. Hypoglycemic episodes – For those on insulin, low blood sugar can occur overnight, causing sweating, confusion, or shakiness. What to do if you notice these signs- Check your blood glucose if you have a meter, especially before bed and after waking. – Consult a healthcare professional for a full evaluation and possible HbA1c test. – Adjust nighttime routines like diet, medication, or hydration based on medical advice. Recognizing these nighttime clues gives you a head start in managing diabetes and preventing complications. If you experience any of these symptoms regularly, seek medical guidance promptly. Do you want a deeper dive into any specific symptom or tips for managing nighttime blood sugar
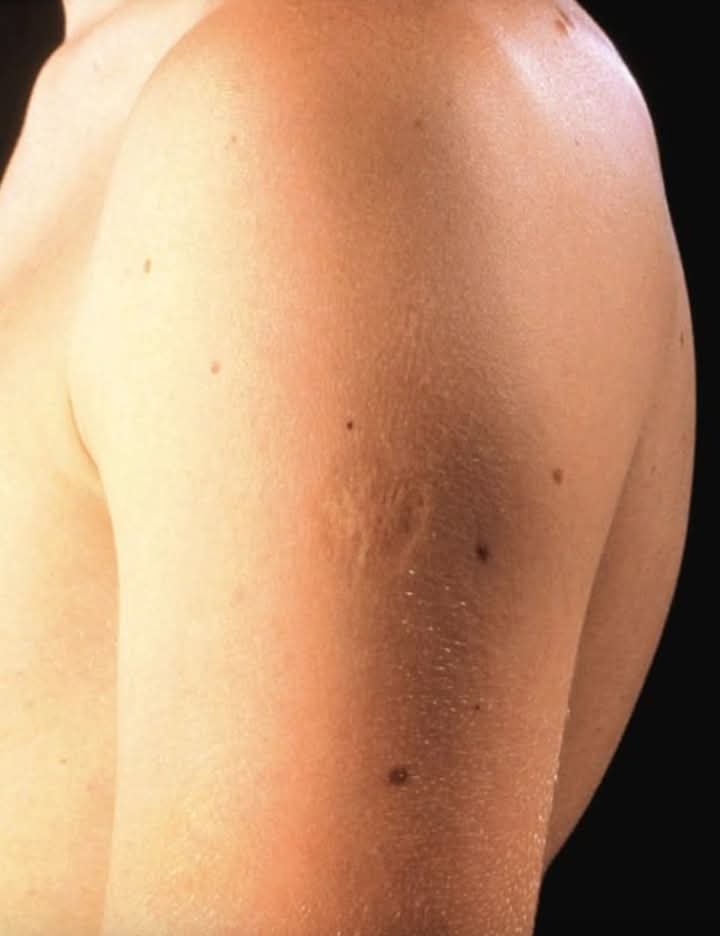
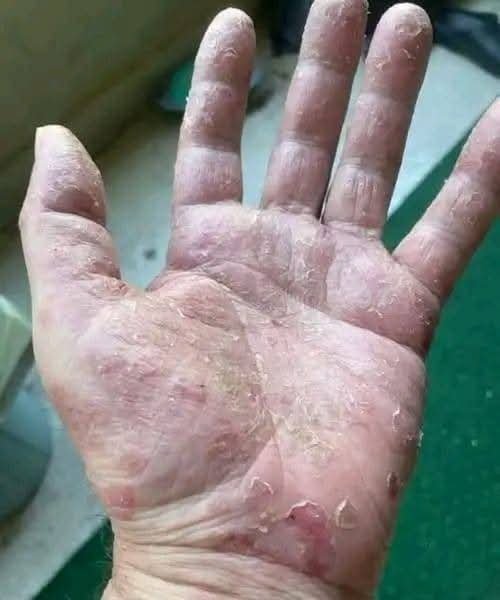
Article: Understanding Severe Hand Skin Peeling (as seen in the photo)
The image shows a hand with severe dryness and peeling skin on the palm and fingers, indicating possible skin irritation or a dermatological condition. c Dry, flaky skin on the palm can be more than just a cosmetic issue; it often signals an underlying problem that needs attention. The peeling shown in the picture suggests excessive loss of the outer skin layer, which can result from environmental factors, skin disorders, or improper skin care. 1. Common causes of palm peeling: – Environmental exposure: frequent hand washing, harsh soaps, chemicals, or extreme weather can strip natural oils, leading to dryness and cracking. – Dermatological conditions: eczema (atopic dermatitis), psoriasis, or contact dermatitis often cause palm scaling and inflammation. – Nutrient deficiencies: lack of vitamins like A, E, or essential fatty acids can affect skin health. 2. Symptoms to watch: – Flaking or shedding of skin in large patches. – Redness, itching, or a burning sensation. – Cracks or fissures that may become painful or infected. 3. Management & treatment: – Moisturize: apply thick emollients or barrier creams immediately after washing and repeatedly throughout the day. – Avoid irritants: use mild, fragrance-free soaps and wear gloves when handling chemicals or during wet work. – Medical care: if symptoms persist, consult a dermatologist for topical steroids, prescription moisturizers, or tests to rule out infections or allergies. 4. Prevention tips: – Keep hands hydrated with regular moisturizing routines. – Use protective gloves for cleaning or gardening. – Maintain a balanced diet rich in vitamins and omega-3 fatty acids for skin health. Severe peeling like in the photo warrants attention to prevent complications such as infections or chronic skin damage. If the condition worsens or causes discomfort, seeking professional dermatological advice is advisable for proper diagnosis and treatment. Do you want more details on specific treatments for hand eczema or tips for choosing the right moisturizer?
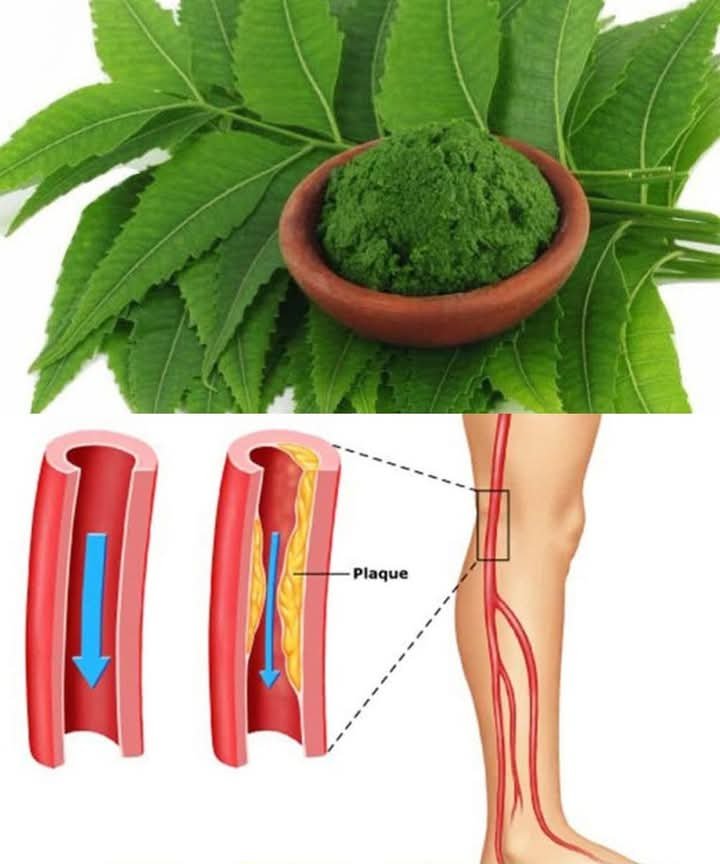
Your legs are screaming “HELP!”: 5 warning signs from your liver…..see more
Liver disease can show up in your legs in a few noticeable ways, often signaling that the liver isn’t functioning properly. When the liver is damaged, it can’t efficiently process toxins and fluids, leading to symptoms that appear in the lower extremities. c